Across much of the world, the high-pitched whine of the mosquito can herald not just an itchy insect bite, but a feverish — and potentially lethal — bout of malaria. Bed nets and insect repellents have reduced opportunities for the bloodsuckers to bite, and in the last two decades, modern medicine finally seemed to have started winning the battle against the disease. Thanks to multinational efforts and major public and private investments, malaria deaths dropped from more than 800,000 in 2000 to fewer than 500,000 in 2015. “There has been incredible progress,” says Audrey Odom John, a pediatrician and malariologist at Washington University in St. Louis.
But lately, malaria rates have begun to creep back up, particularly in sub-Saharan Africa. The World Health Organization estimated that there were about 216 million cases of malaria in 2016 — an increase of 5 million over the previous year. Blood tests that should easily diagnose the disease are missing cases, and therapies that should work within days now take longer.
The estimated global number of deaths from malaria declined between 2010 and 2015, progress that seems to have stalled. Of the nearly half a million malaria deaths that occurred in 2016, approximately 91 percent were in Africa, and none in Europe.
Thanks to extensive public health efforts, malaria rates dropped between 2010 and 2013. They are now on the rise again.
It’s a familiar story, says Odom John. Malaria has been a scourge of humankind for millennia. The disease appears in medical histories going back more than 4,000 years. The malaria parasite, known as Plasmodium, was first identified in the blood of a patient in 1880. In 1897, it was linked to mosquitoes. Since then, humankind, malaria and mosquitoes have been locked in an arms race.
Chinese doctors in the second century BCE used the sweet wormwood plant, Artemisia annua, to treat the disease, and Chinese scientists isolated the active ingredient, artemisinin, from wormwood in 1971. The use of quinine, derived from the bark of the South American cinchona tree, was first recorded by Jesuit missionaries in the early 1600s, and a derivative of quinine called chloroquine was added to the modern antimalaria pharmacopoeia after World War II.

The artemisia, or wormwood, plant is the source of artemisinin, a key antimalarial medication.
CREDIT: VUYCK, L. (1906) FLORA BATAVA / WIKIMEDIA COMMONS
But malaria has fought back. Plasmodium’s genome readily mutates, enabling it to evolve resistance to drugs. Resistance to chloroquine and artemisinin began to develop shortly after the drugs were broadly introduced. For now, artemisinin resistance means the drugs just take longer to clear someone of malaria. But the fear is that such resistance will worsen and spread.
Meanwhile, the mosquitoes that carry the parasite have evolved resistance to pesticides, too. This includes DDT (which was largely responsible for the elimination of malaria in the United States by 1951, but has since been banned in many countries because of its persistence in the environment) and pyrethroids, which remain heavily used in modern antimalaria efforts.
Today, there’s good news and bad news in the global fight against malaria. The World Health Organization announced in June that Paraguay is officially malaria-free; Algeria, Argentina and Uzbekistan are on their way. But many nations are still struggling, points out Jeff Chertack, a senior program officer in global health communications at the Bill & Melinda Gates Foundation in Seattle. His organization has set a goal of eradicating malaria worldwide by 2040.
To consign malaria to the pages of history once and for all will require a smart, multipronged approach. That means new bug sprays. It means better diagnostics, so doctors can identify and treat infections quickly. It means novel drugs. Up-and-coming vaccines may play a role as well.
Keeping mosquitoes at bay
Pesticides that reduce mosquito numbers make a huge difference in malaria incidence. One study attributed 68 percent of the reduction in African malaria cases between 2000 and 2015 to insecticide-treated bed nets. Spraying long-lasting pesticides in homes also helps.
Pyrethroids, the main insecticides used for mosquito control today, interfere with sodium ion channels in the mosquito’s nervous system, paralyzing and eventually killing the pest. However, mosquitoes can evolve ways to survive the toxic stuff. For example, some increase their production of enzymes that can degrade the insecticide.
“There’s pretty much resistance kicking in worldwide,” says Nick Hamon, CEO of IVCC, a nonprofit partnering with insecticide makers to come up with new options.
Even more than drug or diagnostic resistance, pesticide ineffectiveness is the major concern, says Chertack: “It is probably the more clear and present danger, because it’s so widespread.”

A young girl in West Bengal, India, sits in a bed net. Insecticide-treated bed nets, often the first line of defense in protecting people from the mosquitoes that transmit malaria, have played an important role in reducing malaria rates. Now some mosquitoes are starting to resist the pesticides.
CREDIT: JOYDEEP MUKHERJEE / UN DEVELOPMENT PROGRAMME / FLICKR
IVCC and its partners are testing eight compounds as new pesticide candidates, with the aim of providing multiple options.
“We can actually go out with mixtures so we can reduce the probability of resistance,” Hamon explains. Rotating the insecticide in use should also prevent resistance, he says.
Identifying the culprit
The parasite is ultimately the one that brings on malarial fever. Diagnosing malaria can prove challenging, since the disease can look much like other infections. One available tool is a quick blood test that detects a protein in the parasite called HRP2. Between this test and simply examining blood under a microscope, scientists can correctly identify malaria cases 90 percent of the time or more. But Plasmodium doesn’t need HRP2 in order to survive. Some newly evolved parasites lack the HRP2 protein altogether, making them undetectable to the test. These HRP2-negative parasites are showing up in places such as India and Peru, and, according to a recent report, HRP2 tests are missing up to 80 percent of infections in Eritrea.
One new test in development is a cell phone–based microscope that can identify a pigment specific to Plasmodium. Another uses a red light beam that can detect the distinctive look of infected blood cells in a person’s finger.
Odom John has her own new diagnostic platform, inspired by her group’s discovery that the malaria apicoplast — a chloroplast-like cell structure— causes infected blood cells to release chemicals that might attract mosquitoes. These chemicals, called terpenes, mimic those produced by plants.
Odom John found that mosquitoes have smell receptors for these molecules, which might help explain why the insects are especially attracted to people and animals infected with malaria: It seems the parasite actively recruits mosquitoes so it can infect them.
Terpenes easily evaporate into a gas, so Odom John wondered if she could take detect it in a patient’s exhalations. In a study at a clinic in Malawi, she and her collaborators asked 35 children with fevers to blow up a plastic bag. Researchers identified six chemicals at different levels in the 17 children shown to have malaria than in the 18 others. The breathprint test has proved 83 percent accurate in identifying the malaria cases, but still awaits more testing.
“It’s definitely one of the most innovative ideas out there,” says David Fidock, a malariologist at Columbia University Medical Center in New York, who wasn’t involved with the study. Both Fidock and Odom John expect it would be difficult for Plasmodium to evolve invisibility to a breathprint test. The parasite is entirely dependent on mosquitoes to continue its life cycle, so if it stopped making the chemicals that attract the bugs, it presumably would be less likely to reproduce.
A moving target
The very nature of the parasite and its complex life cycle make it a difficult target for scientists and physicians. The Plasmodium parasite is neither a virus nor a bacterium but a single-celled protozoan. Four different species of Plasmodiumcan cause malaria — P. falciparum causes the most severe disease — and the parasites can be transmitted by more than70 different species of mosquito.
When a mosquito bites a person, it transmits the parasite in a form called sporozoites. These infect the liver, where they produce merozoites. Merozoites then infect the person’s red blood cells, causing the disease symptoms: chills and fever, vomiting and diarrhea, sometimes organ failure, coma and even death.
But for malaria parasites to spread, they must infect another mosquito. This requires yet another form: gametocytes. Upon development inside the mosquito gut, new sporozoites emerge, and the cycle continues.
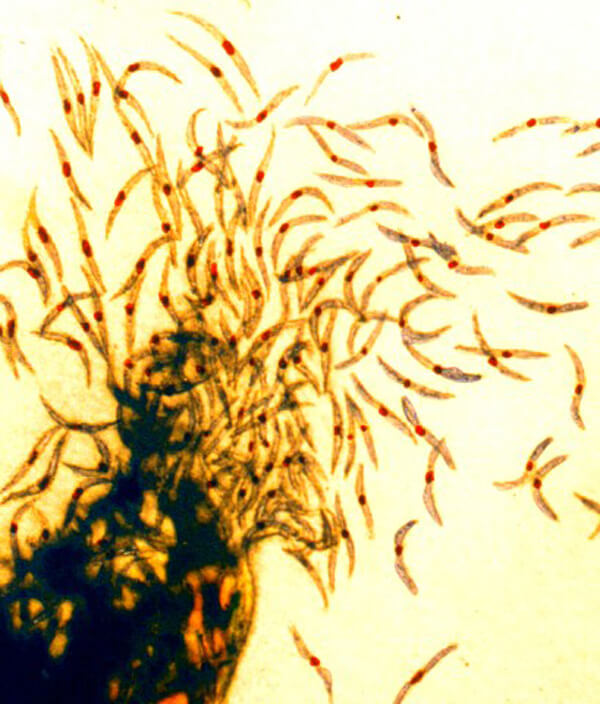
Mosquitoes carry sporozoites, the infectious form of the malaria parasite, which they pass on to people they bite.
CREDIT: NIAID / FLICKR
Further complicating elimination efforts, malaria can evade detection and destruction by a person’s immune system. While immune cells normally learn to recognize and attack repeat invaders, the malaria parasite regularly swaps out the proteins on the surface of infected blood cells, rendering them unrecognizable to the immune system.
Artemisinin combination therapy, the gold standard in malaria treatment since 2001, works by killing both merozoites and some gametocytes. It links two ingredients. First, fast-acting artemisinin (or a derivative) kills many of the parasites in the bloodstream. Since artemisinin only lasts for a few hours in the blood, a second, longer-lasting ingredient, often a quinine derivative, clears away any remaining malaria parasites. The treatment usually involves one or two doses daily for three days. Its use accounts for about 19 percent of the overall decline in malaria cases seen in Africa between 2000 and 2015.
An ounce of prevention
Of course avoiding the disease in the first place would be ideal. Researchers have been experimenting with malaria vaccines for decades. But malaria, with its complex life cycle and propensity to change the look of infected cells, makes vaccine design much trickier than with something like a simple virus, says Brian Greenwood, a biomedical researcher at the London School of Hygiene and Tropical Medicine.
Malaria parasites morph as they go through their various life stages. The parasites jump from humans to mosquitoes as gametocytes, they make the return trip to a human host as sporozoites, and take on different forms in the liver and blood. This makes developing drugs and vaccines tricky.
Today, there are several vaccine candidates under development. The one closest to market is GlaxoSmithKline’s Mosquirix. The injected vaccine trains a recipient’s immune system to recognize and respond to a particular protein that protrudes from the infectious sporozoite. “It’s the best thing that we have evaluated so far,” says Ashley Birkett, who works in Seattle as director of the nonprofit PATH’s Malaria Vaccine Initiative.
In a trial in 11 health centers in sub-Saharan Africa, researchers vaccinated more than 15,000 infants and young children with Mosquirix, and compared their malaria rates over the next three to four years with those of children who had received an unrelated vaccine against rabies or meningococcus. In children aged 5 to 17 months, the vaccine was 28 to 36 percent effective at preventing malaria. In infants aged 6 to 12 weeks, efficacy fell to 18 to 26 percent.
Even though the vaccine failed to protect the majority of children, it could still make a difference in regions where malaria rates run high. “You have to think about the cases of malaria that you’re averting,” Birkett says. Even cutting rates by a third will prevent thousands of cases, he points out. “It’s pretty clear that the vaccine has the potential to have a significant health impact.”
Researchers are planning a pilot release of Mosquirix within the next year, aiming to vaccinate at least 120,000 children each in Ghana, Malawi and Kenya.
Since Mosquirix is the first approved vaccine against malaria — in fact, the first designed for broad human use against any protozoan — there’s a lot of uncertainty about how it will work out in the real world, says Chertack, of the Gates Foundation. “We think there’s going to be a lot to learn from it,” he says, but “it’s definitely, from an effectiveness standpoint, not a silver bullet.”
Greenwood agrees: Mosquirix likely won’t be the last or best vaccine. Another one nearing large-scale testing is under development by Sanaria in Rockville, Maryland; this vaccine is based on disabled Plasmodium sporozoites.
Drug discoveries
Reports of artemisinin drug combination therapies losing efficacy began to emerge in 2002 along the Thailand-Cambodia border. “The drug eventually works,” says Mara Lawniczak, an evolutionary geneticist at the Wellcome Sanger Institute in Hinxton, England. “It’s not full-blown resistance.” But there’s no time to lose, so scientists are looking for new malaria medications that attack the parasites in different ways.
“We want to go beyond just finding replacement drugs,” says Elizabeth Winzeler, a biologist at the University of California San Diego School of Medicine. Because people don’t always take every dose of the artemisinin combination therapy for the necessary three days, Winzeler and other malariologists are trying to come up with drugs that would cure the disease with a single dose. Or ones that would not only kill the merozoites causing symptoms, but also the reproductive forms. Or a prophylactic that would keep people from contracting malaria in the first place.
Winzeler and her colleagues have tested some 1.7 million chemicals to see which could kill the malaria parasite in the lab. In 2008, they reported finding approximately 6,000 potential antimalarials, including several novel ones.
That study led to two new medications now under development by the drugmaker Novartis. One, KAE609, works faster than artemisinin combination therapies and also prevents transmission by gametocytes. It blocks a channel in the parasite’s outer membrane that normally controls its salt and water levels. In one small study, the drug (now called cipargamin) wiped out the parasite in about twelve hours and lasted long enough to be taken just once daily for three days.
Another of Winzeler’s finds, KAF156, not only kills the parasite and transmissible gametocytes in mice, but also acts as a prophylactic, preventing infection by new sporozoites. It’s not certain how KAF156 does it, but the drug has entered human trials.
Also undergoing human testing is MMV390048, developed by researchers at the University of Cape Town in South Africa. It blocks asexual and reproductive life stages in animals by interfering with an enzyme called PI4 kinase, which is involved in a variety of cellular activities.
Another fast-acting artemisinin replacement is OZ439. The drug attacks the merozoites that infect blood cells.
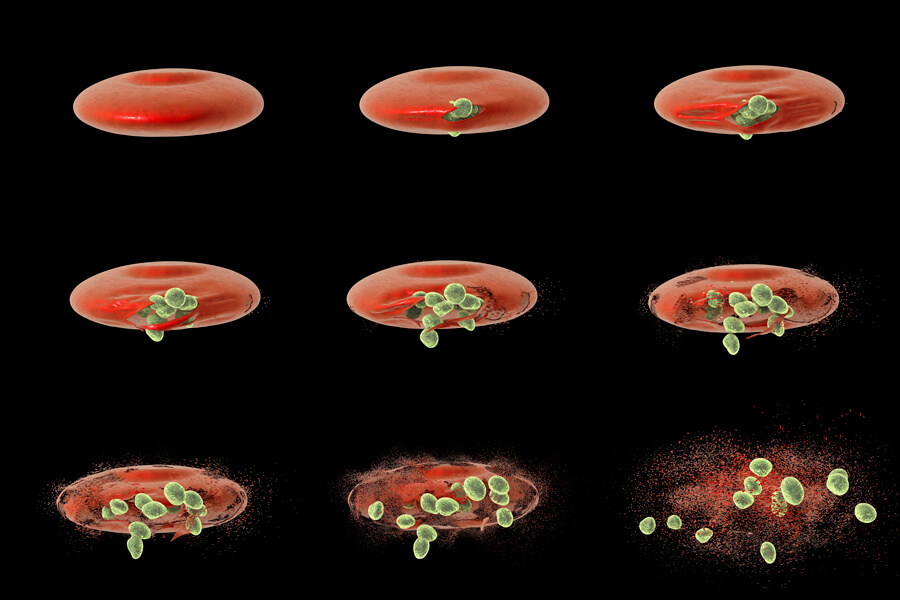
Merozoites infect red blood cells. After they reproduce inside the cells, they burst out of their hosts to invade fresh red blood cells, as shown in this computer illustration.
CREDIT: KATERYNA KON / SCIENCE SOURCE
These four drugs are among the options closest to the market, says Wes Van Voorhis, an infectious disease researcher at the University of Washington in Seattle.
“You need a lot of shots on goal,” says Odom John, since many ideas may not pan out in human studies or real-world situations.
Resisting resistance
What if scientists could come up with a drug that was resistance-proof? “That’s the Holy Grail,” says Dyann Wirth, a parasite biologist at the Harvard T.H. Chan School of Public Health in Boston. “It hasn’t happened for any infectious disease yet.”
That doesn’t mean there’s no hope. Wirth and Winzeler are both part of a consortium working to better understand how resistance evolves, which should provide hints about how to avoid it. In a recent study, the scientists profiled what Winzeler calls the “resistome” — the complement of genes that malaria can alter to protect itself from drugs.
First, they grew P. falciparum in the lab, in the presence of 37 different antimalarial chemicals. The doses weren’t enough to kill all the parasites, but the drugs did select for the parasites that had some natural resistance. The result was 262 different versions of malaria with drug resistance. The researchers then sequenced the microbes’ genes to identify 83 resistance-related genes, including several previously unknown to science. These genes encoded proteins with jobs such as detoxifying or blocking drugs.
Winzeler’s results are exciting, says Odom John, because the team identified the limited number of ways that malaria evolves drug resistance. If scientists can design medicines that interfere with the actions of these genes and proteins in the resistome, the parasite might be less likely to evolve a workaround.
Other researchers are considering drugs based on blue dye, the antibacterial triclosan, anddried wormwood leaves. They’re trying out their ideas in test tubes, mice, people and even computer models.
Some groups are taking aim at mosquitoes with sugary baits to draw them to a toxin-laced meal. And genetic engineers are working to eliminate the disease-causing insects altogether by inserting genes that will drive mosquitoes to extinction.
“We have a suite of imperfect tools,” says Birkett, of PATH, “and if you use a suite of imperfect tools optimally, then you can have substantial public health benefit.”
Others are more hopeful. “We’re attacking the problem in a much more rational sort of way these days,” says Winzeler. “It’s possible you could give it the old one-two punch and get rid of it altogether.”
Within a few decades, she thinks, the mosquito’s whine could be transformed from a harbinger of disease or death to a simple annoyance.
Editor's note: This story was updated September 27, 2018, to correct the name of the Harvard School of Public Health. It is the Harvard T.H. Chan School of Public Health, not Harvard P.H. Chan School of Public Health, as was originally written.




